
Poster #42
Title: iRAM, an AI-based screening tool that redefines the BMI Scale to include Black and Latino Patients in Disease Risk Assessments
Presenting Author: Maya Hatoum
Authors:
Faculty Mentors:
Primary Category: Innovative Solutions to Public Health Challenges
Secondary Category: Health Care, Access to Care, Insurance, Technology
Background: The BMI scale is an outdated and racially biased system that continues to major institutions for defining a healthy body. Using the BMI to assess Patients of Color can not only imply an over/underestimation in weight status, but can also impose a psychological and financial burden on the patient during clinical treatment.
Goal: The purpose of this project is to develop an AI screening tool that rescales BMI markers for Black and Latino patients in disease risk assessments to account for both genetic differences and racial disparities in healthcare.
Objectives: Develop and implement a data model that can estimate risk of weight-related health conditions by analyzing race-specific incidence rates and comparing disease frequency to deviations in waist circumference to height ratios.
Approach/Methods: Tools: SAS software, MS azure. Data model is designed and data is prepared for categorical analysis. Scale is generated based on variable distributions and analyzed for deviations in mean. ICD-10 codes are used to define health conditions while waist-to height circumference is reported as a ratio.
Results: Tool is expected to generate and support findings of genetic differences and racial disparities and confirm the importance of assessing BMI values that are race-specific to Black and Latino communities.
Importance to Public Health: This tool will assist physicians in making more informed decisions concerning diagnosis and treatment of obesity and cardiovascular diseases for ethnic groups who are not being represented on the current health metric scale.
Poster # 50
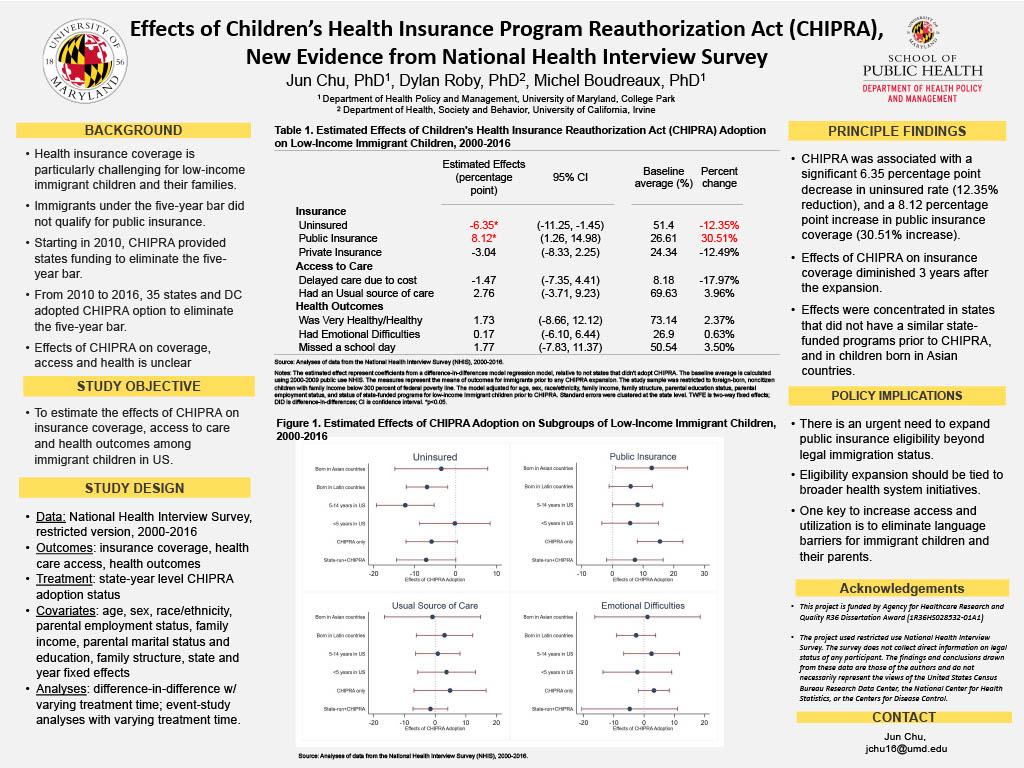
Title: Effects of Children’s Health Insurance Program Reauthorization Act (CHIPRA), New Evidence from National Health Interview Survey
Presenting Author: Jun Chu
Authors: Dylan Roby, PhD, Department of Health, Society and Behavior, University of California, Irvine; Michel Boudreaux, SPH Faculty
Faculty Mentors: Michel Boudreaux
Primary Category: Health Care, Access to Care, Insurance, Technology
Secondary Category: Healthy Equity, Racism and Social Injustice, Population Health, Immigration and Health
Background: Health insurance coverage is particularly challenging for low-income immigrant children and their families. Starting in 2010, CHIPRA provided states funding to eliminate the five-year bar.
Goal: To estimate the effects of CHIPRA on insurance coverage, access to care and health outcomes among immigrant children in US.
Objectives: To estimate the effects of CHIPRA on insurance coverage, access to care and health outcomes among immigrant children in US.
Approach/Methods: Difference-in-differences with varying treatment time.
Results: CHIPRA was associated with a significant 6.35 percentage point decrease in uninsured rate (12.35% reduction), and a 8.12 percentage point increase in public insurance coverage (30.51% increase). Effects of CHIPRA on insurance coverage diminished 3 years after the expansion. Effects were concentrated in states that did not have a similar state-funded programs prior to CHIPRA, and in children born in Asian countries.
Importance to Public Health: There is an urgent need to expand public insurance eligibility beyond legal immigration status. Eligibility expansion should be tied to broader health system initiatives. One key to increase access and utilization is to eliminate language barriers for immigrant children and their parents.
